
12
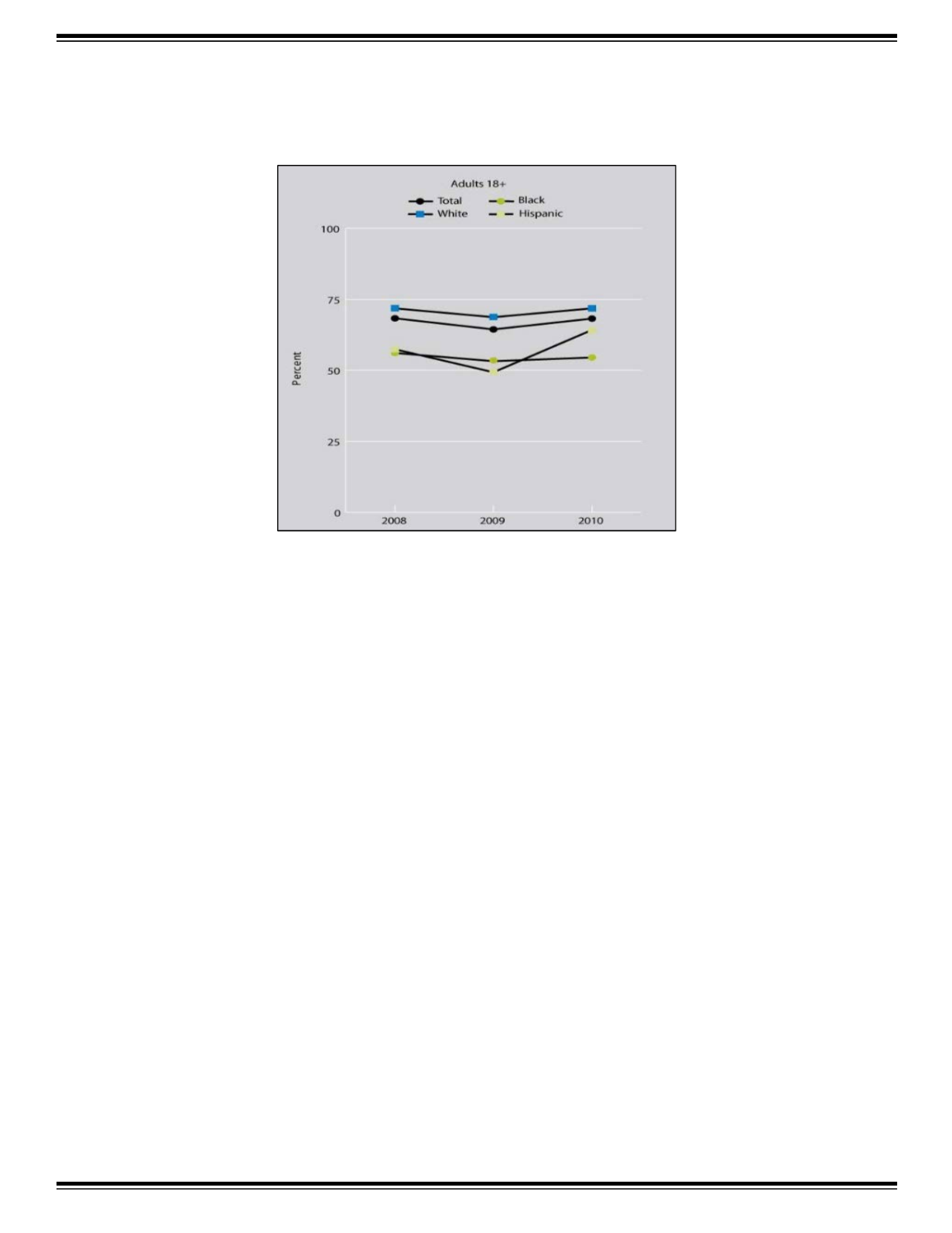
depression, as published in the 2012 National Healthcare Disparities Report (NHDR). In all years, African American and
Hispanic adults were less likely to receive treatment for depression than Caucasian American adults.
Figure 4: Adults Who Experienced Major Depression and Treatment within the Same Year by Race/Ethnicity,
2008 – 2010
Figure 6: Adults Who Experienced Major Depression and Treatment within the Same Year
by Race/Ethnicity, 2008 – 2010
Source:
Substance Abuse and Mental Health Services Administration, National Survey on Drug Use and Health, 2008-2010.
A 2007 Science Update, by the National Institute of Mental Health (NIMH), referenced a special
issue of
Research in Human Development
, published in the same year that examined then current
trends in prevalence and risk factors for mental health disorders across the lifespan in diverse U.S.
minority populations.
24, 25
Notable findings from the special issue showed that of the more than
2,554 Latinos interviewed for the National Latino and Asian American Study (NLAAS), age at time
of immigration was a factor in the mental health of this diverse minority population. According to
Margarita Alegría, PhD.,
et.al., in general, the older the person at immigration, the later the onset of
psychiatric disorders. Those who arrived later in life had lower lifetime prevalence rates than
younger immigrants or U.S. born Latinos. However, after about age 30, the risk of depressive
disorders increased among these later-arriving Latino immigrants, whereas risk tended to decrease
between ages 30-40 for U.S. born Latinos and immigrants arriving before age seven. Latinos
arriving between ages 0-6 had very high risks of onset shortly after immigration, but after several
years, their lifetime prevalence rates approached those of Latinos born in the United States.
25
According to a NIMH-funded analysis published in the American Journal of Public Health in 2011,
older racial and ethnic minorities are less likely to be diagnosed with depression than their
Caucasian counterparts, but are also less likely to get treated once they are diagnosed.
26
Ayse Akincigil Ph.D,
et.al., found that about 6.4% of Caucasian American patients, 4.2% of African
Americans, and 7.2% of Hispanics were diagnosed with depression. Among those diagnosed,
73% of Caucasian Americans received treatment (either with antidepressants, psychotherapy or
both); while 60% of African Americans received treatment and 63.4% of Hispanics received
treatment. These kinds of diagnosis and treatment differences are consistent with previous studies,
the researchers noted. Although they noted pronounced differences in socioeconomic status and
Source:
Substance Abuse and Mental Health Services Administration, National Survey on Drug Use and Health, 2008-2010.
A 2007 Science Update, by the National Institute of Mental Health (NIMH), referenced a special issue of
Research in
Human Development
, published in the same year that examined then current trends in prevalence and risk factors for
mental health disorders across the lifespan in diverse U.S. minority populations.
24, 25
Notable findings from the special issue
showed that of the more than 2,554 Latinos interviewed for the National Latino and Asian American Study (NLAAS), age
at time of immigration was a factor in the mental health of this diverse minority population. According to Margarita Alegría,
PhD.,
et.al., in general, the older the person at immigration, the later the onset of psychiatric disorders. Those who arrived
later in life had lower lifetime prevalence rates than youn
ger immigrants or U.S. born Latinos. However, after about age 30,
the risk of depressive disorders increased among these later-arriving Latino immigrants, whereas risk tended to decrease
between ages 30-40 for U.S. born Latinos and immigrants arriving before age seven. Latinos arriving between ages 0-6 had
very high risks of onset shortly after immigration, but after several years, their lifetime prevalence rates approached those of
Latinos born in the United States.
25
According to a NIMH-funded analysis published in the American Journal of Public Health in 2011, older racial and ethnic
minorities are less likely to be diagnosed with depression than their Caucasian counterparts, but are also less likely to get
treated once they are diagnosed.
26
Ayse Akincigil Ph.D,
et.al., found that about 6.4% of Caucasian Am rican patients, 4.2% of African Am rican , and 7.2%
of Hispanics were diagnosed with depression. Among hose diagno ed, 73% of Caucasian Ameri ans received treatment
(either with antidepressants, psychotherapy or both); while 60% of African Americans received treatment and 63.4% of
Hispanics received treatment. The kinds of diagno
sis and treatment differences are consistent with previous studies, the
researchers noted. Although they noted pronounced differences in socioeconomic status and quality of insurance coverage
across ethnicities, these differences did not appear to account for the disparities in diagnosis or treatment rates.
The significance of these findings is consistent with the notion that depression continues to be under-recognized and
undertreated among older minoriti s. According to the researchers, future investigation should explore cultural factors, such
as help-seeking patterns, stigma, and patient attitudes and knowledge about depression as potential aspects contributing to
the disparities.



















