
13
THE LINK BETWEEN PAIN AND DEPRESSION
Major depression can be associated with painful physical symptoms such as
headache, backache, stomachache, joint ache, and muscle ache. Because
depression and pain share a common neuro-chemical pathway in that
they are both influenced by serotonin and norepinephrine, depression and
associated painful physical symptoms must be treated together in order
to achieve remission.
27
In fact, research has shown that improvement of
physical symptoms was correlated with the improvement of other depression
symptoms, which
suggests that the patient’s ability to achieve depression
remission may be directly
28
related to the reduction of painful physical symptoms.
People with prolonged pain have three times the average risk of developing psychiatric symptoms, usually mood or anxiety
disorders. Physical symptoms are common in depression and vague aches and pain are often the presenting symptoms of
depression.
27
Studies have shown that depressed patients have three times the average risk of developing chronic pain.
28
It
is a complex experience because pain is depressing, and depression causes and intensifies pain.
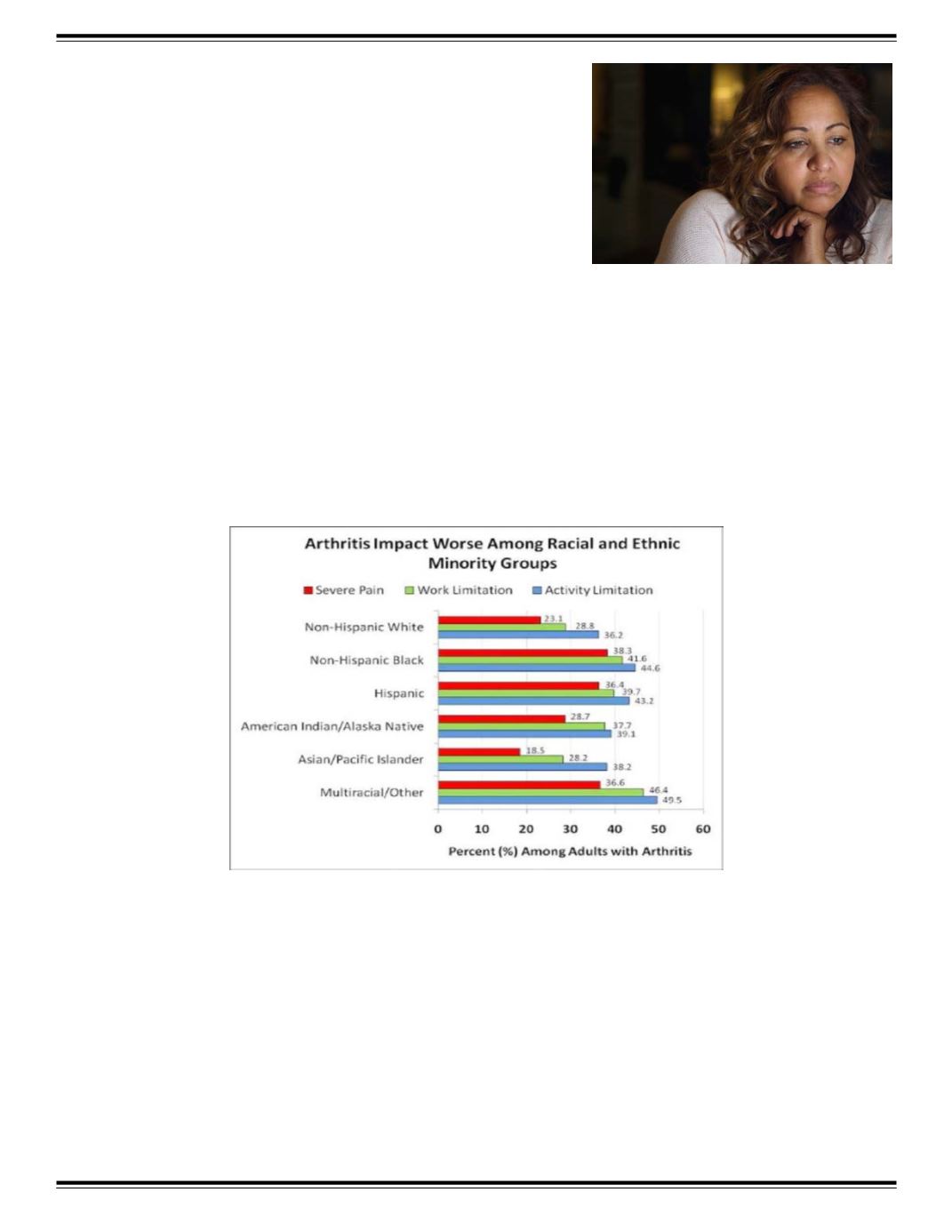
This is especially significant because in a 2010 issue of Preventing Chronic
Disease, the CDC reported that compared with Caucasian Americans, African Americans and Hispanic/Latino Americans
have higher rates of activity limitation and severe pain related to arthritis.
Figure 5: Arthritis Impact Worse among Racial and Ethnic Minority Groups
Dr. Patricia A. Parmelee, et. al., conducted a cross-sectional study, published in 2012, that examined how race and sex
affects associations among OA pain, disability, and depression. The study included 363 African American and Caucasian
adults who self-reported pain, disability and depressive symptoms. The results of the study revealed that women
experienced greater pain and marginally greater disability than men. At a deeper level, African American women reported
greater disability and marginally greater pain than Caucasian women.
30
In a study of 130,880 people from the Canadian Community Health Survey, it was found that those with arthritis experienced
twice the rate of major depression and suicidal thoughts as those who didn’t have the disease.
31
In a study by Louise B. Murphy,
et.al., the primary objective was to estimate the prevalence and correlation of anxiety and
depression among US adults (ages ≥45 years old) with doctor-diagnosed arthritis (n = 1,793) from the Arthritis Conditions
Health Effects Survey. Anxiety and depression were measured using separate and validated subscales of the Arthritis
Impact Measurement Scales. Prevalence was estimated for the sample overall and stratified by subgroups.
32



















