
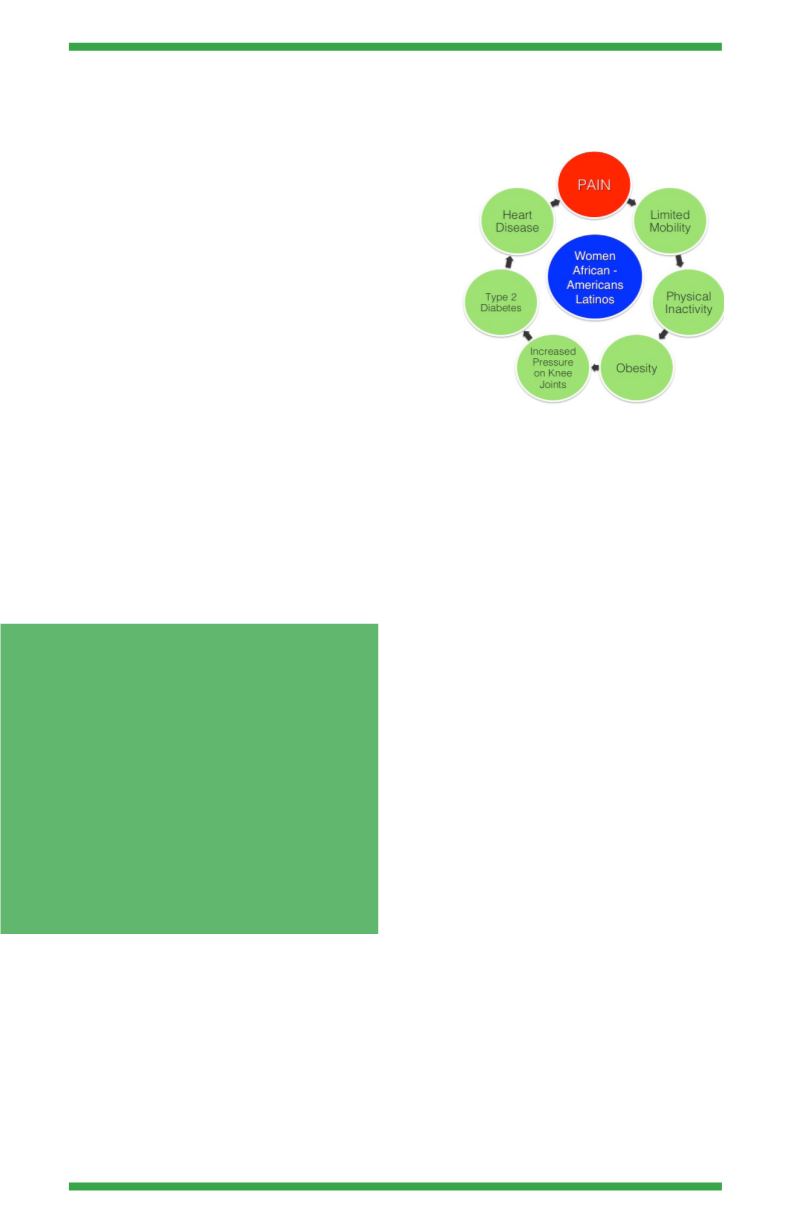
21
OA.
62
Randomized controlled interventions of diet, exercise, and diet plus exercise among
overweight and obese adults with osteoarthritis have reduced body weight by approximately
5%, improving symptoms and functioning, and preventing short-term disability.
55
A study by the CDC of 1973 US adults ages ≥ 45
years with doctor-diagnosed arthritis found that one-
third of respondents reported having either anxiety,
depression, or both. Anxiety was found to be
almost twice as common as depression (31% and
18%, respectively). Given their high prevalence,
their profound impact on quality of life, and the
range of effective treatments available, the authors
encourage healthcare providers to screen all people
with arthritis for both anxiety and depression.
63
As the largest occupational group in health care
delivery, nurses can be a force in changing how OA is perceived and managed. Healthcare
providers have an opportunity to discuss how even modest weight loss and physical activity,
including exercise, decreases pain, improves function, and boosts mood.
64
Self-directed
low-impact activities, such as walking and swimming are effective, as are community-based
physical activity classes. People with arthritis often worry that exercise will exacerbate joint
symptoms, but if that happens, it is short-lived and benefits are evident within days to weeks
of starting an exercise program.
O
f those diagnosed with osteo-
arthritis,
52
%
have diabetes,
57
%
have heart disease, and
53
%
have hypertension. Physical
activity is essential for managing
these chronic co-morbid conditions.

















